Paneth cells: Maestros for the microbes
- Alex Cloherty
- May 27, 2019
- 4 min read
Today on Microbial Mondays, we are giving a shoutout to some particular cells in your GI tract that play a very special role in the health of your gut. These cells, which hang out in your “intestinal crypts”, or the little valleys in between the long cilia in your intestinal tract, are called Paneth cells.
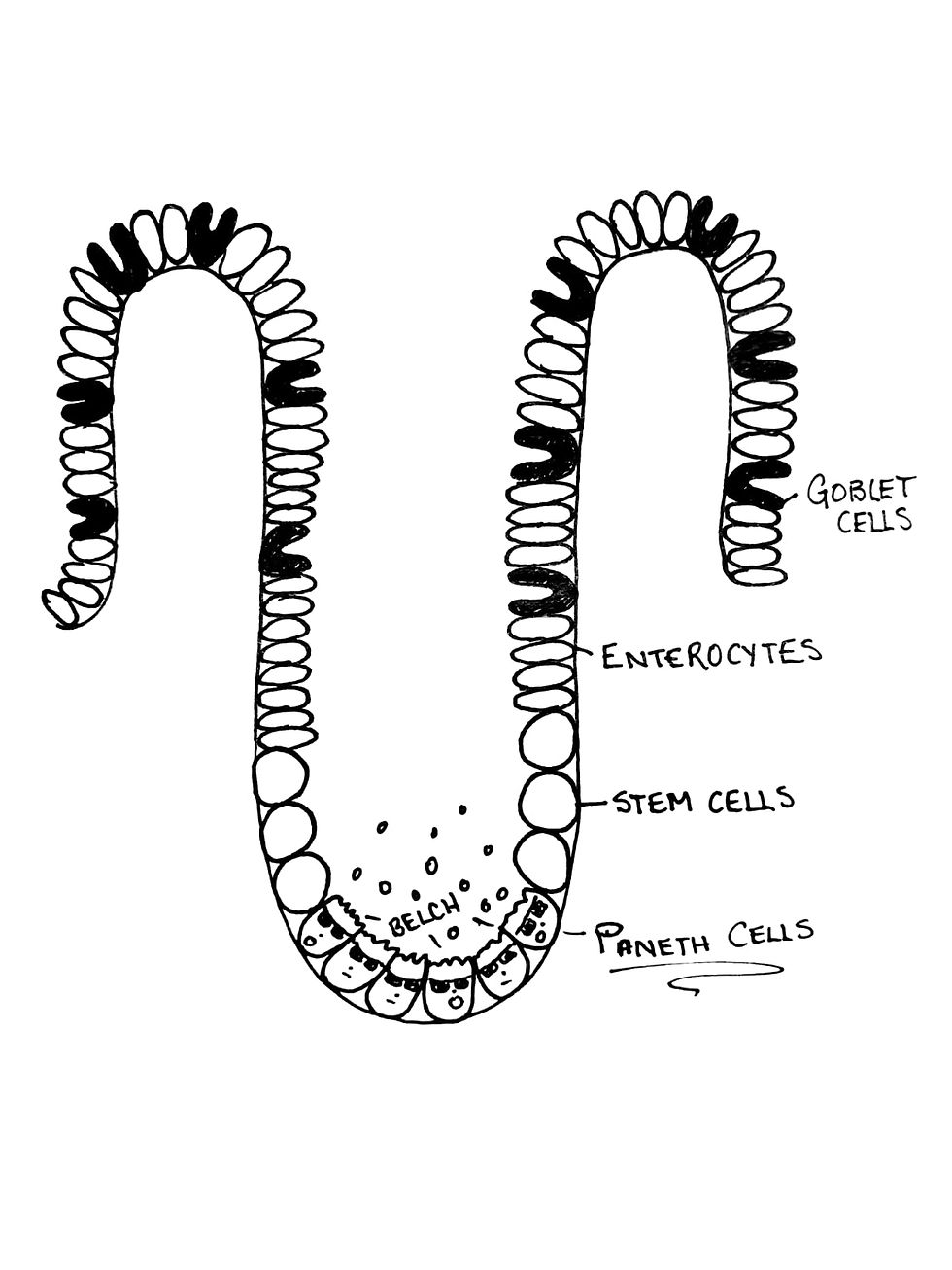
When I first heard the name of these cells, I thought it was a play on the prefix “pan-“, which basically means “all”, like in the Greek panacea. I figured this was a homage to their all-important role as “maestros of the intestinal crypts”, as one paper put it. Let’s back up a step – what are these crypts, and why are they important? Intestinal crypts are tiny, tiny glands in your small and large intestines that contain a bunch of different cells that all help with digestion. In these crypts live goblet cells, which release mucous into the intestine, so-called “enterocytes”, which absorb nutrients, stem cells which help regenerate damaged intestine, and – of course – paneth cells.
It turns out, as I found out today, that paneth cells were not intentionally given a name that alludes to their maestro-like functioning. Rather, they took the name of their discoverer. Joseph Paneth was an Austrian doctor who first identified the cells. I had never heard of the man himself before, probably because he died at only age 33, but he made a great discovery at his young age. But, let’s get back to the cells themselves. You probably remember that the bacteria within your intestine are very important for your overall health. To give a quick recap, they help you digest your food, provide you with nutrients, and help keep you safe from invading pathogens (i.e. “bad bugs”). But how do we keep these microbial buddies in our guts under control? Paneth cells are one of the answers to this questions.
Paneth cells are “professional secretors”: they are basically cells that are specialized for throwing up stuff into your intestines. And what exactly are they throwing up? Perhaps the most important category of paneth-puke contents is a group of proteins called “antimicrobial peptides”. Antimicrobial peptides are small proteins that can be found across pretty much all multicellular organisms, from plants to praying mantises to people. These little proteins help us all fight off unwanted microbes, acting more or less as self-made antibiotics.
When paneth cells spit out antimicrobial peptides, they help support the delicate balance that exists between our own cells and our microbial buddies in our intestines. Studies in animals have shown that antimicrobial peptides thrown up by paneth cells don’t only kill the bad bacteria, but they seem to somehow help the good ones, too. We’re not yet totally sure how this works, but we do know that if paneth cells aren’t working so well, the makeup of the population of microbes in the gut totally changes.
You can imagine this like the multicultural population in Vancouver. At different times throughout history, the composition of the population has changes. At one time there were mostly Indigenous peoples living there, and then white Caucasians, and now (according to the latest data I could find) about one third of the population has Chinese heritage. This has changed over time, and according to many different interconnected factors. Something similar can happen in your gut. The composition of different microbes can change, depending on both the situation in your gut (“Vancouver”) and in your environment (“the Earth as a whole”). Now we know that the antimicrobial peptides being thrown up by paneth cells are kind of like immigration officers.
Now, let’s step away from that potentially politically charged analogy and get back to the straight-up science. Why exactly is it important to regulate the microbes in your intestine? We can get some insight into this by looking at Crohn’s disease.
In a healthy human gut, the “bad” bacteria are limited, and the “good bacteria” not only thrive, but also help inform the human immune system. They help the human immune system within the gut learn to tolerate the “good” microbial buddies, and let them live peacefully rather than targeting them as dangerous intruders. However, when paneth cells stop working properly and no longer puke out normal amounts of antimicrobial peptides, which helps keep the microbial population under control, this delicate balance is upset. The immune system gets confused because of the changes in the microbial population, and then worried that there are pathogens (“bad” bacteria) intruding, and then starts to freak out. In immunological terms, “freaking out” means massive inflammation. This massive inflammation is meant to help get the microbial population back under control, but it can also accidentally damage the human cells as well as the microbes. This damage of human cells within your intestine can then send more signals to your immune system that something is wrong, which then triggers more inflammation, which then can damage more human cells… and you get the picture.
This downward spiral of inflammation, tissue damage, and more inflammation can get worse and worse, until the inflammation won’t go away any more. And that stubborn inflammation is basically what we call Inflammatory Bowel Disease (IBD), of which Crohn’s disease is a subtype.
So, now you have the downside of poorly functioning paneth cells. But, we can also learn a lot from properly functioning paneth cells! For one, if we look at the differences between how paneth cells work in healthy people versus people with inflammatory diseases like IBD, we can potentially learn about how to treat the disease. In addition, if we zoom in and look just at antimicrobial peptides, we can find a wealth of information.
You might have heard about the current problems concerning antimicrobial resistance. If you haven’t, please do read more about it here, since it is a very important topic for all of us to stay healthy! Antimicrobial resistance is perhaps the biggest, scariest problem faced by modern medicine. However, antimicrobial peptides give us some hope. Scientists are currently studying antimicrobial peptides produced by all sorts of different living things all along the tree of life, in order to learn “design principles” from these proteins that could be applied to develop new antibiotics.
So, to sum up, what have we learned from the paneth cells? Everybody pukes.
Until next week – I hope you have a settled stomach ;)
~Alex
PS. If you found this interesting and want to dive more into the science, this is an excellent paper to read over! Enjoy.




Comments